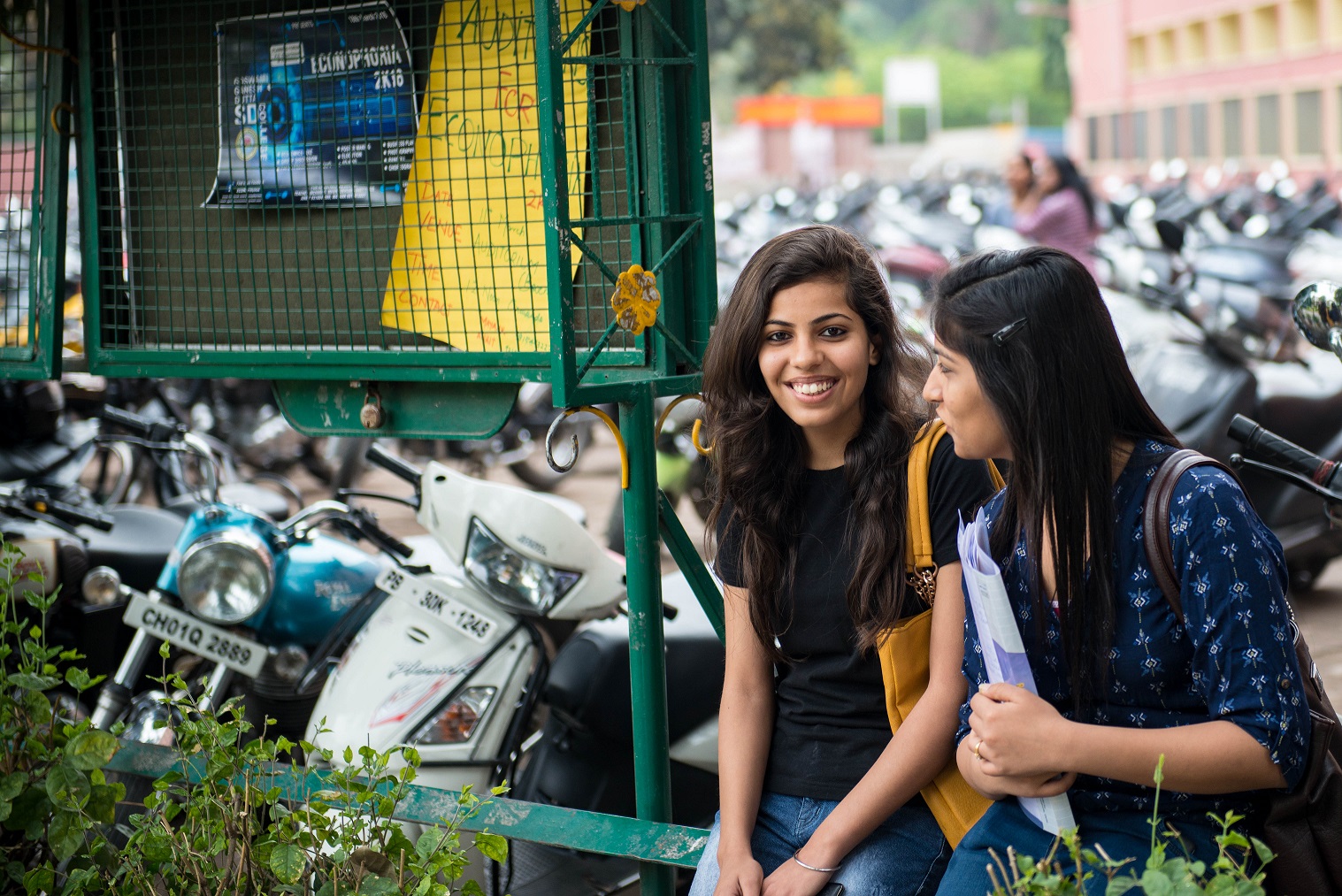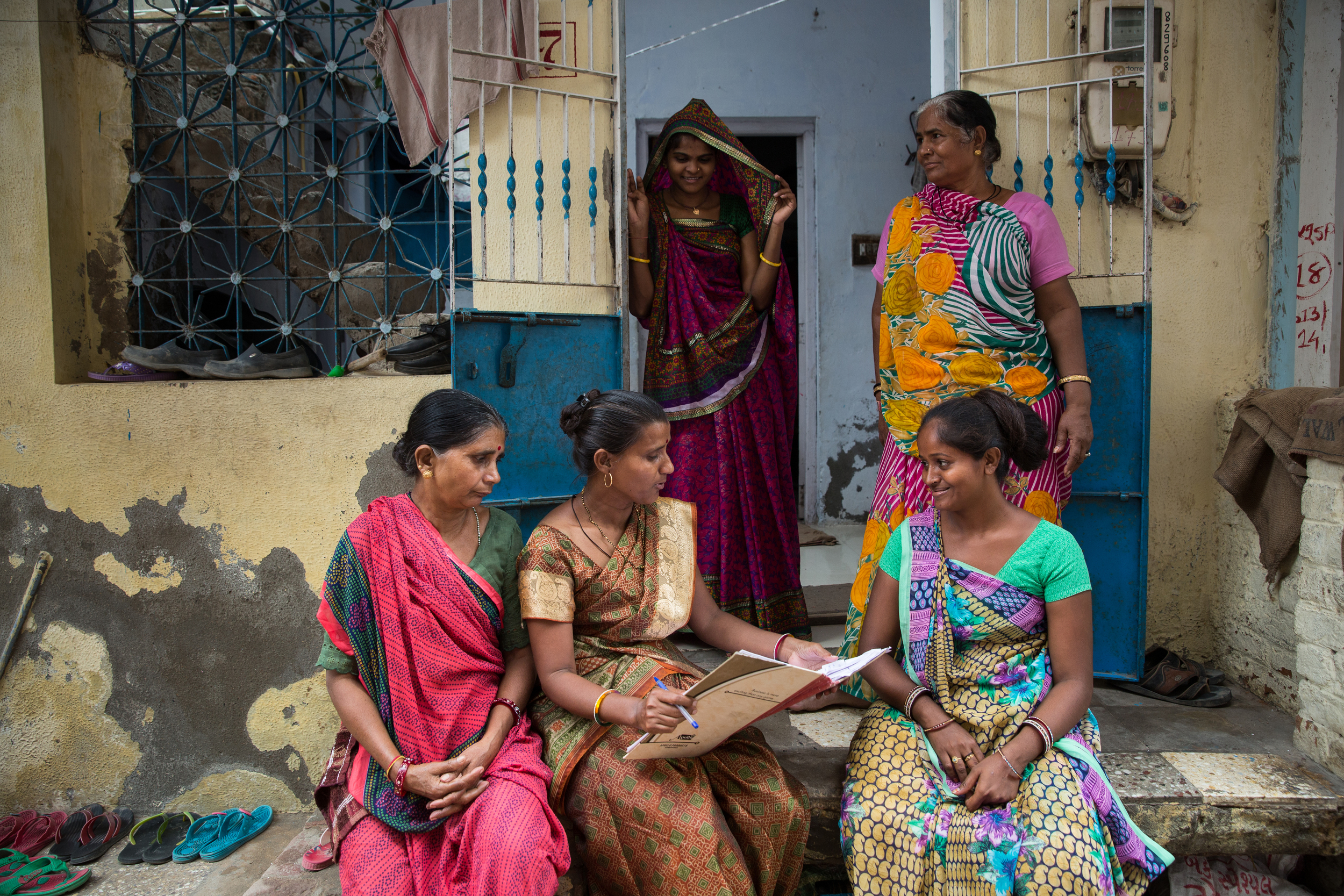View the latest family planning advocacy news from our partners.
On September 30, 2019, government officials from Assam, Bihar, Jharkhand, Maharashtra, Rajasthan and Uttar Pradesh committed to expanding access to quality family planning by sustaining local advocacy working groups. They made the commitments during a commemoration seminar held by the Advance Family Planning initiative and its partners, Foundation for Reproductive Health Services India, Jhpiego, Pathfinder International, and Population Foundation of India, to mark five years of advocacy achievements.
Intrauterine device (IUD) acceptance rates rose among postpartum women following a series of improvements to the quality of family planning services provided in four districts in Assam state. Postpartum IUD insertions in 25 facilities increased to 7.8% of all deliveries following the improvement of services (March 2018 to April 2019), compared to just 1.4% of deliveries before them (August 2017 to February 2018)[1].
Twenty-six public health facilities in Ahmednagar district in Maharashtra, India, have seen a 26% increase in the number of clients receiving postpartum intrauterine device (PPIUD) services between April 2018 and March 2019, compared to the same period last year. This increase in uptake follows renewed government efforts to enhance provider training on family planning counseling and PPIUD service delivery across the district. Acceptance rates for PPIUD among clients delivering in facilities also rose 8 percentage points from 25.4% to 33.4%, compared to the prior year.
On September 27, 2018, the Governing Board of the State Innovations in Family Planning Services Project Agency (SIFPSA)[1] approved a proposal to establish youth centers in 40 colleges across Uttar Pradesh. The proposal included a budget of 14.8 million Indian rupees (INR) (US $207,500) and an operational plan for all 18 divisions in the state.
In June, the Government of India earmarked $409,470 to expand its “Ensuring Spacing at Birth” scheme across all 34 districts in Maharashtra. Advocates initially sought to extend the effort into one district, but incited a larger advocacy movement for state-wide expansion. Consequently, the scheme allocation for Maharashtra state is a sevenfold increase (646%) from the previous year’s budget of $54,899.
Barpeta, Darrang, Dhubri, and Morigaon districts in the state of Assam, India are beginning to see results after establishing a comprehensive mechanism to provide family planning counselling and services for eligible couples in public health facilities.
The Jhansi district of Uttar Pradesh, India strengthened 11 facilities to provide quality female sterilization services between May and October 2017, eight of which began providing the services for the first time. Fixed day services (FDS) ensure that quality female sterilization services are available on a designated day every week, all year long rather, than only during particular months of the year.
Twenty-five health sub-centers in the Sitapur district of Uttar Pradesh, India that initiated fixed day services (FDS) for intra-uterine device (IUD) services are beginning to see results. Uptake of IUDs increased 30-fold, from 20 insertions between July 2016 and June 2017 to 685 insertions between July 2017 and June 2018.
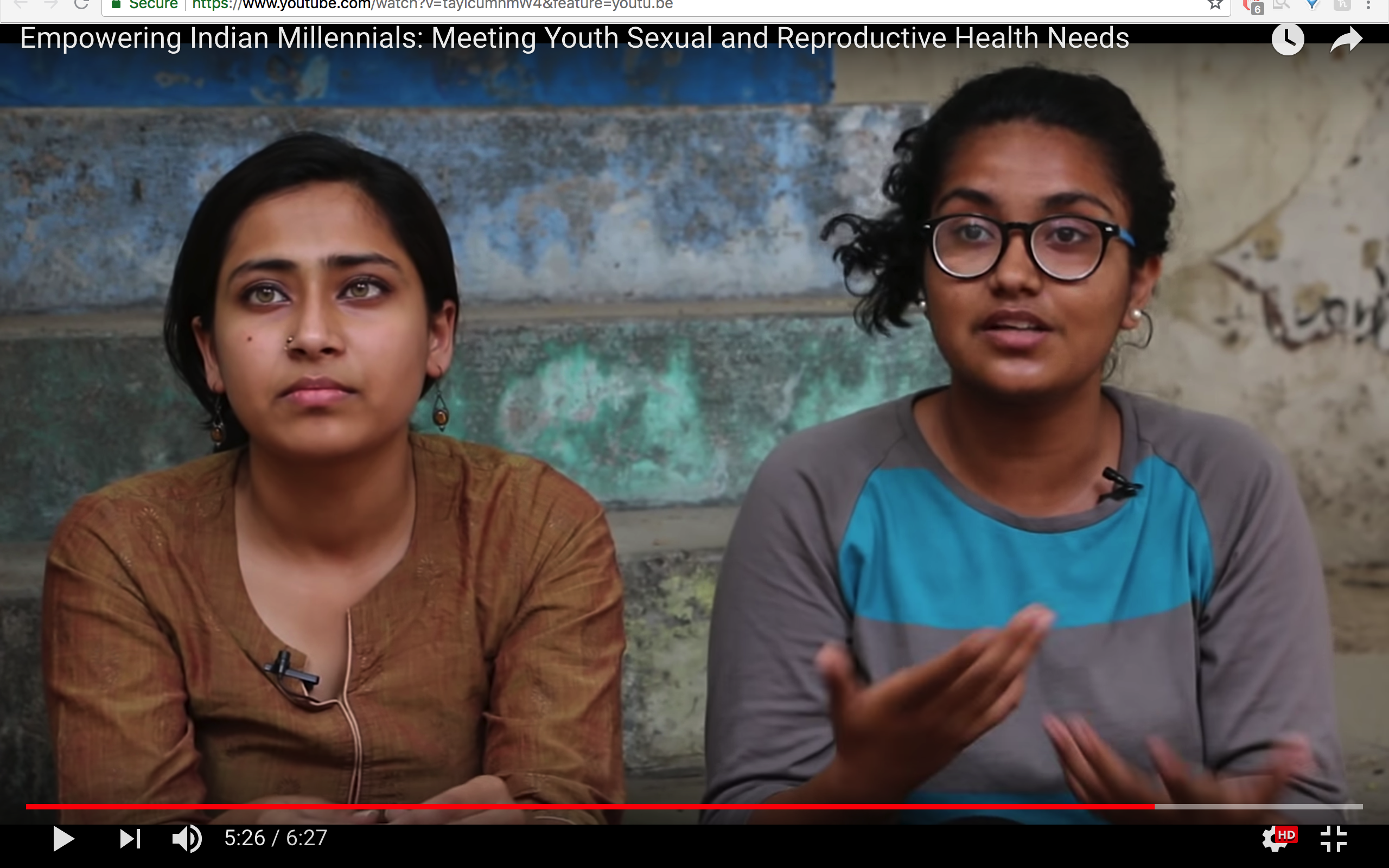
Advance Family Planning (AFP) local partner Jhpiego India, in collaboration with Population Reference Bureau, launched a new video[1] and factsheet[2] entitled
After a year-long gap without replenished family planning supplies, India’s Uttar Pradesh state Director of Family Welfare and Health enabled the supply of commodities in the Mau district. In December 2017, Mau and two additional districts from the Azamgarh Division were supplied with approximately 1.5 million condoms, 140,000 packets of oral contraceptive pills, 48,900 pregnancy testing kits, and 14,500 falope rings used for sterilization. Moreover, a smoother process with oriented stakeholders will allow for regular replenishment.
Between December 2017 and January 2018, 13 private health facilities and clinics in Uttar Pradesh’s Sultanpur district began providing free family planning counseling and services on one day every month. The services include provision of intrauterine devices (IUDs), condoms, and oral contraceptive pills. Private health facilities and clinics typically provide these services at a cost to clients.
The National Health Mission, India approved a total increased budget of 45.1 million Indian Rupees (INR) (US $688,000) for developing and procuring information, education, and communication (IEC) materials and postpartum intrauterine device (IUD) insertion forceps in Maharashtra state’s budget for fiscal year 2017-2018.